TDH Employee Experience Initiatives
Improving Employee Experience & Retention at TimeDoc Health
TimeDoc faced two critical challenges:
- A high turnover rate—many new Care Coordinators (CCs) quit within their first 60 days
- Workflow inconsistencies that slowed daily patient calls and affected care quality
My role
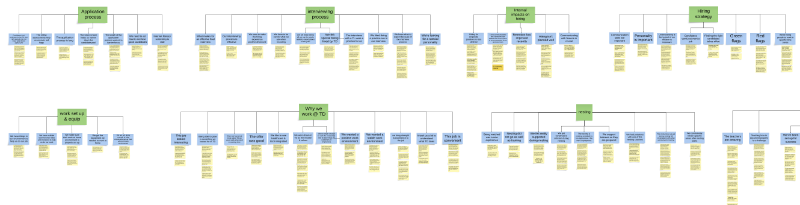
Partnering with HR, QA, and recruiting, I led two research initiatives. I interviewed and observed CCs, mapped their task flows, and uncovered patterns in both workplace setup and onboarding experiences. These insights revealed where breakdowns occurred—and why some CCs thrived while others left.
The result
- Introduced persona-based hiring to better match candidates with role expectations
- Streamlined onboarding, reducing early turnover
- Identified the most effective workspace layouts and task sequencing to boost daily output